 At what point does waiting compromise the visual outcome? 
It’s clear the patient needs surgery to repair the retinal detachment, but how quickly does this need to occur? Does it need to be done on the same day (that we diagnosed the retinal detachment) or can it wait until the next day or even the day after? This becomes particularly important in the era of COVID-19, where surgical patients must be tested for the virus and negative prior to surgery. It is believed that these irregular focal adhesions are responsible for a majority of retinal tears not associated with lattice degeneration. This, in turn, may result in isolated areas of focal traction on the retina that may result in the development of a horseshoe tear. Through the natural aging process, the vitreous begins to liquefy, and irregularities develop in the shape and extent of where it attaches to the retina. The adhesion of the vitreous at the peripheral retina is usually evenly distributed circumferentially. It measures about 2mm to 6mm wide and straddles the ora serrata. The base represents a circumferential zone where the vitreous is attached to the peripheral retina. Horseshoe tears most commonly develop as a result of traction at the posterior margin of the vitreous base. That is clearly what has occurred in our patient. Why did she develop a retinal tear after already having had a PVD? The assumption is that every tractional force occurring on the retina is relieved after developing a PVD, but that’s not always the case because the vitreous can still be attached anteriorly, causing traction. 
There are a few interesting questions to consider. Despite being macula-off, visual acuity was surprisingly good, which likely indicates that the macula has not been off for very long. In fact, the macula may still be on temporally, but it is clearly off superiorly where we can see fluid and separation of the retinal from the RPE. The OCT confirms the macula is off, but just barely. A retinal tear can be seen along the superior temporal arcade. Our patient has a macula-off rhegmatogenous retinal detachment. How do you interpret this OCT scan through the macula? Click image to enlarge. What is the likely visual outcome at this point?įig. What is the time frame that this needs to be treated before it affects the final visual outcome?ĥ. Surgical retinotomy and gas fluid exchangeĤ. Injection of gas and laser photocoagulationĭ. Pars plana vitrectomy (PPV), endo laser and possible scleral buckle procedure (SBP)Ĭ. Chronic retinal detachment with subretinal fibrosisĢ. What does this finding represent? Click image to enlarge.ĭ. This is the widefield fundus photo of the left eye of our patient. OCT was performed and is available for review ( Figure 2). There were obvious fundus changes ( Figure 1). In the left eye, a PVD was also present in addition to pigment cells in the anterior vitreous. The anterior segment examination was unremarkable.įundus examination of the right eye was normal. 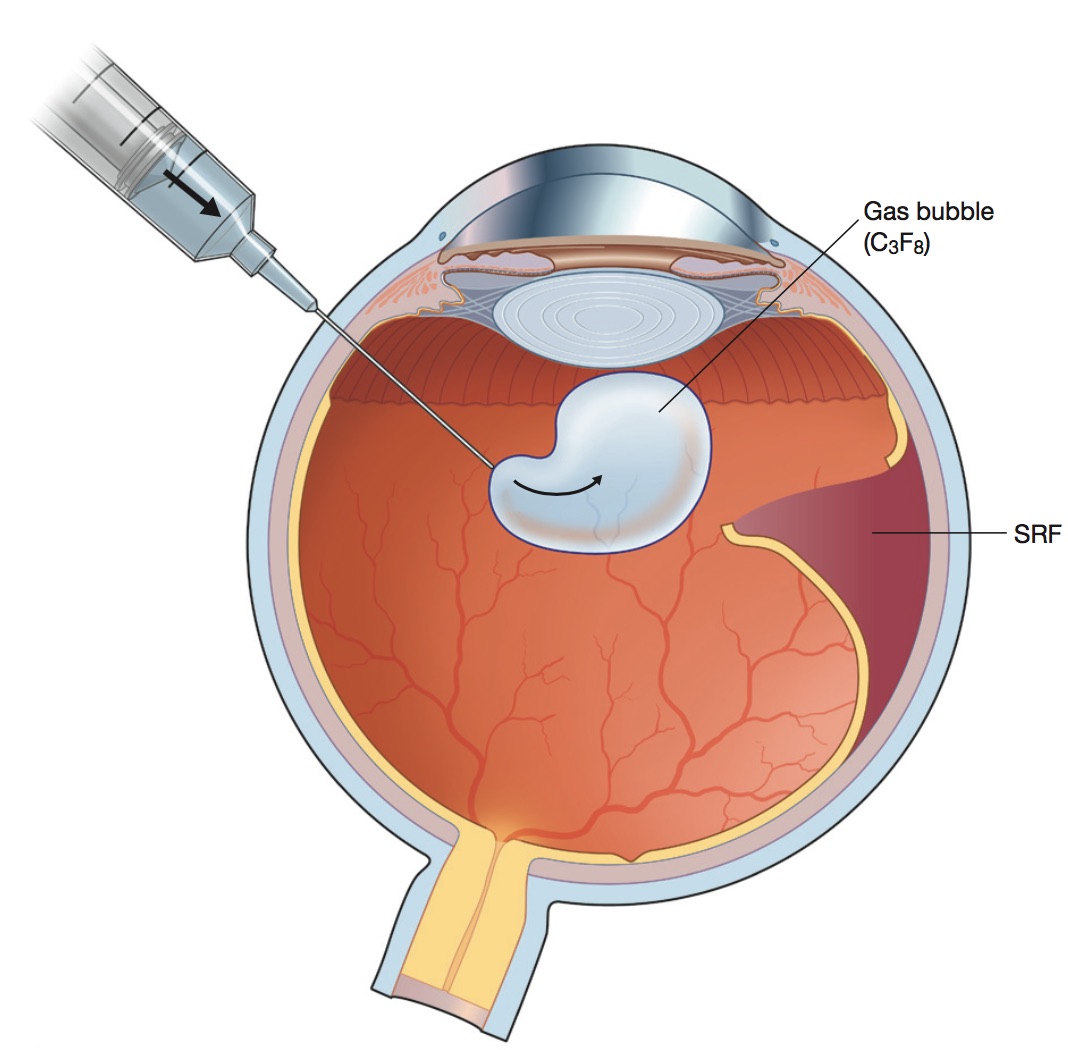
Her pupils were equally round and reactive to light there was no afferent pupillary defect. Confrontation visual fields were full-to-careful finger counting OU. On this most recent examination, her best-corrected visual acuity measured 20/20 OD and 20/40 OS. Besides the PVDs, her retinal exam was unremarkable. At that visit, she was noted to have resolving Bell’s palsy on the right side and posterior vitreous detachment (PVD) in both eyes. A review of her medical record showed that she had been seen almost 18 months prior. The message was read the next day, and she came in two days later. A 66-year-old female established patient sent a message via her electronic health review saying she started seeing a new onset of floaters in her left eye for the past four days and wanted to know if she should be seen in-person for an eye exam. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
